Acute Respiratory Failure, Pediatric
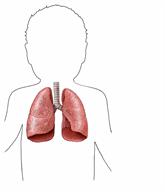
Acute respiratory failure is when one or both of these things happen:
Oxygen cannot pass from the lungs into the blood, causing the blood oxygen level to drop. Loss of blood oxygen means tissues and organs may not work well.
A gas called carbon dioxide cannot pass from the blood into the lungs so the body can get rid of it. The buildup of carbon dioxide can damage the tissues and organs in the body.
Acute respiratory failure is a condition that happens fast. It is an emergency and needs to be treated right away.
What are the causes?
Common causes of respiratory failure that may cause low oxygen levels include:
Trauma to the lung, chest, or ribs, or to the tissues around the lung.
Lung conditions, such as asthma, bronchiolitis, or pneumonia.
Breathing in harmful chemicals, smoke, water, or vomit.
A widespread infection (sepsis).
Common causes of respiratory failure that cause a buildup of carbon dioxide include:
What increases the risk?
This condition is more likely to develop in children who:
Were born early (preterm birth).
Have lung diseases such as bronchopulmonary dysplasia (BPD), asthma, or cystic fibrosis (CF).
Have a condition that damages or weakens the muscles, nerves, bones, or tissues that are involved in breathing, such as muscular dystrophy.
Have a health problem that blocks the unconscious reflex that is involved in breathing, such as hypothyroidism or sleep apnea.
What are the signs or symptoms?
Symptoms may depend on the cause and on the levels of oxygen and carbon dioxide in your child's blood.
Trouble breathing is the main symptom of acute respiratory failure.
Other symptoms may include:
Fast breathing, making high-pitched whistling sounds when breathing (wheezing), or grunting.
Flaring of the nostrils.
A fast heartbeat.
Sleeping more than normal or being hard to wake.
Not being able to play or do normal activity.
Skin, lips, or fingernails that look blue (cyanosis).
Fussiness, anxiety, or confusion.
How is this diagnosed?
This condition may be diagnosed based on:
How is this treated?
This condition is usually treated in a hospital intensive care unit (ICU). Treatment depends on the cause of the condition. Treatment may include one or more of these:
Oxygen given through your child's nose, a face mask, or a hood.
A device to help your child breathe, such as a continuous positive airway pressure (CPAP) machine or bilevel positive airway pressure (BIPAP) machine. The device gives your child oxygen and pressure.
Other breathing treatments, fluids, and medicines.
A breathing machine (ventilator). This machine gives your child oxygen and pressure. A tube is put into your child's mouth and windpipe (trachea) and connects to the ventilator. This treatment offers more control over your child's breathing.
Follow these instructions at home:
Medicines
-
Give over-the-counter and prescription medicines only as told by your child's health care provider.
-
If your child was prescribed antibiotics, give them as told by the health care provider. Do not stop giving the antibiotic even if your child starts to feel better.
-
Do not give your child aspirin because of the association with Reye's syndrome.
General instructions
-
Have your child return to normal activities as told by the health care provider. Ask the health care provider what activities are safe for your child.
-
Do not allow your child to use any products that contain nicotine or tobacco. These products include cigarettes, chewing tobacco, and vaping devices, such as e-cigarettes. If your child needs help quitting, ask a health care provider.
-
Do not smoke around your child.
-
Keep all follow-up visits.
Contact a health care provider if:
-
Your child is having trouble breathing.
-
Your child loses consciousness.
-
Your child's heart starts beating very fast
-
Your child's fingers, lips, or other areas of the body turn blue.
-
Your child becomes confused.
-
Your child who is younger than 3 months has a temperature of 100.4°F (38°C) or higher.
-
Your child who is 3 months to 3 years old has a temperature of 102.2°F (39°C) or higher.
These symptoms may be an emergency. Do not wait to see if the symptoms will go away. Get help right away. Call 911.
Summary
-
Acute respiratory failure is a condition that develops fast and needs to be treated right away.
-
The main symptom of this condition is trouble breathing.
-
This condition is usually treated in a hospital intensive care unit (ICU). Treatment may include oxygen, fluids, and medicines. A ventilator or other device may be used to help your child breathe.
-
Contact your child's health care provider if your child's symptoms do not improve or if they get worse.
This information is not intended to replace advice given to you by your health care provider. Make sure you discuss any questions you have with your health care provider.
 Acute respiratory failure is when one or both of these things happen:
Acute respiratory failure is when one or both of these things happen: This condition may be diagnosed based on:
This condition may be diagnosed based on: