Allergies, Pediatric
An allergy is a condition that causes the body's defense system (immune system) to react too strongly to an allergen. An allergen is a substance that is harmless to most people but can cause a reaction in some people.
Allergies often affect the nose (allergic rhinitis), eyes (allergic conjunctivitis), skin (atopic dermatitis), and stomach. They can be mild, moderate, or severe. They cannot spread from person to person. Allergies can start at any age. In some cases, they may go away as your child gets older.
What are the causes?
Allergies are caused by allergens. These may be:
Outdoor allergens. These include pollen, car fumes, and mold.
Indoor allergens. These include dust, smoke, mold, and pet dander.
Other allergens. These include foods, medicines, scents, and insect bites or stings.
What increases the risk?
Your child is more likely to have allergies if they have:
Family members with allergies.
Family members who have a condition that may be caused by allergens, such as asthma.
What are the signs or symptoms?
Symptoms depend on how severe the allergy is.
Mild to moderate symptoms
-
Runny nose, stuffy nose (nasal congestion), or sneezing.
-
Itchy mouth, ears, or throat.
-
Postnasal drip. This is a feeling of mucus dripping down the back of your child's throat.
-
Sore throat.
-
Itchy, red, watery, or puffy eyes.
-
Skin rash, or itchy, red, swollen areas of skin (hives).
-
Stomach cramps or bloating.
Severe symptoms
A bad allergy to food, medicine, or insect bites may cause a severe allergic reaction (
anaphylactic reaction). Symptoms include:
A red face.
Coughing or high-pitched whistling sounds when your child breathes out (wheezing).
Swollen lips, tongue, or mouth.
A tight or swollen throat.
Chest pain or tightness, or a fast heartbeat.
Trouble breathing or shortness of breath.
Pain in the abdomen.
Vomiting or diarrhea.
Feeling dizzy or fainting.
How is this diagnosed?
Allergies are diagnosed based on your child's symptoms, family and medical history, and a physical exam. Your child may also have tests, such as:
You may be asked to:
How is this treated?
Treatment for allergies depends on your child's age and symptoms. It may include:
Cold, wet cloths (cold compresses). These can be used to soothe itching and swelling.
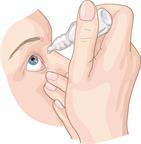
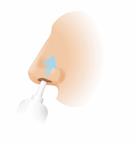
Eye drops or nasal sprays.
A saline solution to clear out your child's nose and keep it moist (nasal irrigation). A saline solution is made of salt and water.
A humidifier. This can add moisture to the air.
Skin creams. These can treat rashes or itching.
Diet changes to cut out foods that cause allergies.
- Exposing your child again and again to tiny amounts of allergens. This can help your child's body build a defense against the allergens (tolerance). The process is called immunotherapy. It may be done using:
Allergy medicines (antihistamines) or other medicines. These can help block the allergic reaction.
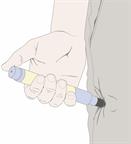
Using an auto-injector pen. An auto-injector pen is a device filled with medicine that gives an emergency shot of epinephrine. The health care provider will teach you how to give the shot.
Follow these instructions at home:
Medicines
-
Give or apply over-the-counter and prescription medicines only as told by your child's provider.
-
Have your child always carry an auto-injector pen if they are at risk of an anaphylactic reaction. Give your child the shot as told by the provider.
Eating and drinking
General instructions
-
Have your child wear a medical alert bracelet or necklace if they have had an anaphylactic reaction in the past.
-
Help your child avoid known allergens.
-
Talk with your child's school staff and caregivers about your child's allergies and how to prevent them. Make a plan that includes what to do if your child has a severe reaction.
-
Keep all follow-up visits. The provider will watch your child's symptoms and talk about treatment options.
Contact a health care provider if:
-
Your child has symptoms of anaphylaxis.
-
You have to use the auto-injector pen on your child. Your child will need more medical care even if the medicine seems to be working. An anaphylactic reaction may happen again within 72 hours (rebound anaphylaxis).
These symptoms may be an emergency. Do not wait to see if the symptoms will go away. Use the auto-injector pen right away. Then, call 911.
This information is not intended to replace advice given to you by your health care provider. Make sure you discuss any questions you have with your health care provider.