Managing Your Hypertension
Hypertension, also called high blood pressure, is when the force of the blood pressing against the walls of the arteries is too strong. Arteries are blood vessels that carry blood from your heart throughout your body. Hypertension forces the heart to work harder to pump blood and may cause the arteries to become narrow or stiff.
Understanding blood pressure readings
A blood pressure reading includes a higher number over a lower number:
The first, or top, number is called the systolic pressure. It is a measure of the pressure in your arteries as your heart beats.
The second, or bottom number, is called the diastolic pressure. It is a measure of the pressure in your arteries as the heart relaxes.
For most people, a normal blood pressure is below 120/80. Your personal target blood pressure may vary depending on your medical conditions, your age, and other factors.
Blood pressure is classified into four stages. Based on your blood pressure reading, your health care provider may use the following stages to determine what type of treatment you need, if any. Systolic pressure and diastolic pressure are measured in a unit called millimeters of mercury (mmHg).
Normal
Elevated
Hypertension stage 1
Hypertension stage 2
How can this condition affect me?
Managing your hypertension is very important. Over time, hypertension can damage the arteries and decrease blood flow to parts of the body, including the brain, heart, and kidneys. Having untreated or uncontrolled hypertension can lead to:
What actions can I take to manage this condition?
Hypertension can be managed by making lifestyle changes and possibly by taking medicines. Your health care provider will help you make a plan to bring your blood pressure within a normal range. You may be referred for counseling on a healthy diet and physical activity.
Nutrition

Lifestyle

-
Work with your health care provider to maintain a healthy body weight or to lose weight. Ask what an ideal weight is for you.
-
Get at least 30 minutes of exercise that causes your heart to beat faster (aerobic exercise) most days of the week. Activities may include walking, swimming, or biking.
-
Include exercise to strengthen your muscles (resistance exercise), such as weight lifting, as part of your weekly exercise routine. Try to do these types of exercises for 30 minutes at least 3 days a week.
-
Do not use any products that contain nicotine or tobacco. These products include cigarettes, chewing tobacco, and vaping devices, such as e-cigarettes. If you need help quitting, ask your health care provider.
-
Control any long-term (chronic) conditions you have, such as high cholesterol or diabetes.
-
Identify your sources of stress and find ways to manage stress. This may include meditation, deep breathing, or making time for fun activities.
Alcohol use
-
Do not drink alcohol if:
Your health care provider tells you not to drink.
You are pregnant, may be pregnant, or are planning to become pregnant.
- If you drink alcohol:
- Limit how much you have to:
Know how much alcohol is in your drink. In the U.S., one drink equals one 12 oz bottle of beer (355 mL), one 5 oz glass of wine (148 mL), or one 1½ oz glass of hard liquor (44 mL).
Medicines
Your health care provider may prescribe medicine if lifestyle changes are not enough to get your blood pressure under control and if:
Take medicines only as told by your health care provider. Follow the directions carefully. Blood pressure medicines must be taken as told by your health care provider. The medicine does not work as well when you skip doses. Skipping doses also puts you at risk for problems.
Monitoring
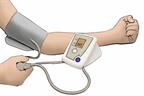
Before you monitor your blood pressure:
Do not smoke, drink caffeinated beverages, or exercise within 30 minutes before taking a measurement.
Use the bathroom and empty your bladder (urinate).
Sit quietly for at least 5 minutes before taking measurements.
Monitor your blood pressure at home as told by your health care provider. To do this:
Sit with your back straight and supported.
Place your feet flat on the floor. Do not cross your legs.
Support your arm on a flat surface, such as a table. Make sure your upper arm is at heart level.
Each time you measure, take two or three readings one minute apart and record the results.
You may also need to have your blood pressure checked regularly by your health care provider.
General information
Talk with your health care provider about your diet, exercise habits, and other lifestyle factors that may be contributing to hypertension.
Review all the medicines you take with your health care provider because there may be side effects or interactions.
Keep all follow-up visits. Your health care provider can help you create and adjust your plan for managing your high blood pressure.
Contact a health care provider if:
-
You think you are having a reaction to medicines you have taken.
-
You have repeated (recurrent) headaches.
-
You feel dizzy.
-
You have swelling in your ankles.
-
You have trouble with your vision.
-
You develop a severe headache or confusion.
-
You have unusual weakness or numbness, or you feel faint.
-
You have severe pain in your chest or abdomen.
-
You vomit repeatedly.
-
You have trouble breathing.
These symptoms may be an emergency. Get help right away. Call 911.
Summary
-
Hypertension is when the force of blood pumping through your arteries is too strong. If this condition is not controlled, it may put you at risk for serious complications.
-
Your personal target blood pressure may vary depending on your medical conditions, your age, and other factors. For most people, a normal blood pressure is less than 120/80.
-
Hypertension is managed by lifestyle changes, medicines, or both.
-
Lifestyle changes to help manage hypertension include losing weight, eating a healthy, low-sodium diet, exercising more, stopping smoking, and limiting alcohol.
This information is not intended to replace advice given to you by your health care provider. Make sure you discuss any questions you have with your health care provider.


 Before you monitor your blood pressure:
Before you monitor your blood pressure: