Middle Ear Infection (Otitis Media) in Children: What to Know
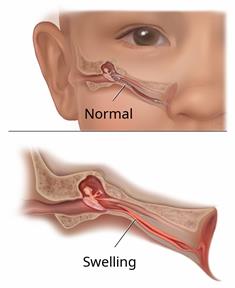
Otitis media happens when there's swelling (inflammation) and fluid in the middle ear, showing signs of an infection. The middle ear is a part of the ear that has bones used for hearing as well as air that helps send sounds to the brain.
When infected fluid builds up in the middle ear, it causes pressure and results in an ear infection. The eustachian tube is a small tube that connects the middle ear to the back of the nose. It normally allows air into the middle ear and drains fluid from the middle ear. If this tube becomes blocked, fluid can build up and cause an infection.
What are the causes?
Otitis media is caused by a blockage in the eustachian tube. This can be caused by mucus or by swelling of the tube. Problems that can cause a blockage include:
Allergies.
Colds and other infections that affect the nose, throat, or airways.
Enlarged areas of soft tissue high in the back of the throat, behind the nose and the roof of the mouth.
A swelling or growth of cells (mass) in the back of the nose.
Changes in air pressure that happen fast, like when a plane descends.
What increases the risk?
Your child is more likely to get otitis media if they're younger than 7 years old. Before age 7, a child's ear is shaped in a way that can cause fluid to collect in the middle ear. This makes it easier for germs like bacteria or viruses to grow. Also, children this age don't have as strong a defense against germs as older children and adults do.
Your child may also be more likely to get otitis media if:
They have repeated ear and sinus infections or a family history of these.
They have problems in their body's defense system (immune system).
They have acid reflux or have an opening in the roof of their mouth.
They attend day care.
They weren't breastfed.
They're exposed to tobacco smoke.
They take a bottle while lying down or use a pacifier.
What are the signs or symptoms?
Symptoms include:
Children too young to speak may show other signs, such as:
Tugging, rubbing, or holding the ear.
Crying more than usual.
Irritability.
Not eating as much as usual.
Trouble sleeping.
How is this diagnosed?
Otitis media is diagnosed with a physical exam. Your child's health care provider will use a tool called an otoscope to look in your child's ear. They will also ask about your child's symptoms.
Your child may have tests, including:
How is this treated?
Otitis media may go away on its own. If your child needs treatment, the exact treatment will depend on your child's age and symptoms. It may include:
Waiting 48–72 hours to see if your child's symptoms get better.
Medicines for pain. These may be given by mouth or put in the ear.
Antibiotics. These may be given if your child's condition is caused by bacteria.
A minor surgery to insert small tubes into your child's eardrums. This may be needed if your child has many ear infections within several months. The tubes help drain fluid and prevent infection.
Follow these instructions at home:
-
Give your child medicines only as told.
-
If your child was given antibiotics, give the antibiotics as told. Do not stop giving the antibiotics even if your child starts to feel better.
How is this prevented?
-
Keep your child away from irritants such as tobacco smoke.
-
Keep your child's ears clean and dry.
-
Avoid feeding your child while they're lying down.
Contact a health care provider if:
-
Your child's hearing seems to get worse.
-
Your child's symptoms don't get better, or they get worse, after 2–3 days.
Contact your child's provider right away if:
Your baby is younger than 3 months old and has a temperature of 100.4°F (38°C) or higher.
Your child is 3 months old or older and has a temperature of 102.2°F (39°C) or higher.
Your child has a fever, and they look or act sick in a way that worries you.
If you can't reach the provider, go to an urgent care or emergency room.
-
Your child has a headache.
-
Your child has neck pain or a stiff neck.
-
Your child seems to have very little energy.
-
Your child has a lot of watery poop (diarrhea).
-
Your child throws up a lot.
-
The bone behind your child's ear is sore.
-
The muscles of your child's face don't seem to move.
This information is not intended to replace advice given to you by your health care provider. Make sure you discuss any questions you have with your health care provider.
