Rheumatoid Arthritis
Rheumatoid arthritis (RA) is a long-term (chronic) disease that causes inflammation in the joints. RA may start slowly. It most often affects the small joints of the hands and feet. Usually, the same joints are affected on both sides of the body. Inflammation from RA can also affect other parts of the body, including the heart, eyes, or lungs.
There is no cure for RA, but medicines can help your symptoms and stop or slow down the progression of the disease.
What are the causes?
RA is an autoimmune disease. When you have an autoimmune disease, your body's defense system (immune system) mistakenly attacks healthy body tissues. The exact cause of RA is not known.
What increases the risk?
The following factors may make you more likely to develop this condition:
Being female.
Having a family history of RA or other autoimmune diseases.
Having a history of smoking.
Being obese.
Having been exposed to pollutants or chemicals.
What are the signs or symptoms?
Symptoms of this condition usually start gradually. They are often worse in the morning. The first symptom may be morning stiffness that lasts longer than 30 minutes.
As RA progresses, symptoms may include:
Pain, stiffness, swelling, warmth, and tenderness in joints on both sides of your body.
Loss of energy.
Loss of appetite.
Weight loss.
Low-grade fever.
Dry eyes and dry mouth.
Firm lumps (rheumatoid nodules) that grow beneath your skin in areas such as your forearm bones near your elbows and on your hands.
Changes in the appearance of joints (deformity) and loss of joint function.
Symptoms of this condition vary from person to person.
Symptoms of RA often come and go.
Sometimes, symptoms get worse for a period of time. These are called flares.
How is this diagnosed?
This condition is diagnosed based on your symptoms, medical history, and a physical exam. You may have X-rays or an MRI to check for the type of joint changes that are caused by RA.
You may also have blood tests to look for:
How is this treated?
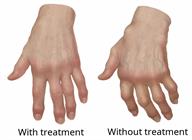
The goals of treatment are to relieve pain, reduce inflammation, and slow down or stop joint damage and disability. Treatment may include:
Lifestyle changes. It is important to rest as needed, eat a healthy diet, and exercise.
- Medicines. Your health care provider may adjust your medicines every 3 months until treatment goals are reached. Common medicines include:
Pain relievers (analgesics).
Corticosteroids and NSAIDs, such as ibuprofen, to reduce inflammation.
Disease-modifying antirheumatic drugs (DMARDs) to try to slow the course of the disease.
Biologic response modifiers to reduce inflammation and damage.
Physical therapy and occupational therapy.
Surgery, if you have severe joint damage. Joint replacement or fusing of joints may be needed.
Your health care provider will work with you to identify the best treatment option for you based on assessment of the overall disease activity in your body.
Follow these instructions at home:
Managing pain, stiffness, and swelling
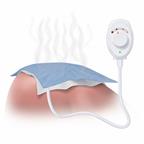
If directed, apply heat to the affected area as often as told by your health care provider. Use the heat source that your health care provider recommends, such as a moist heat pack or a heating pad.
Place a towel between your skin and the heat source.
Leave the heat on for 20–30 minutes.
Remove the heat if your skin turns bright red. This is especially important if you are unable to feel pain, heat, or cold. You have a greater risk of getting burned.
Activity
-
Return to your normal activities as told by your health care provider. Ask your health care provider what activities are safe for you.
-
Rest when you are having a flare.
-
Start an exercise program as told by your health care provider. This may include physical therapy exercises to maintain movement and strength in your joints.
General instructions
Contact a health care provider if:
-
You have chest pain.
-
You have trouble breathing.
-
You quickly develop a hot, painful joint that is more severe than your usual joint aches.
These symptoms may be an emergency. Get help right away. Call 911.
Summary
-
Rheumatoid arthritis (RA) is a long-term (chronic) disease that causes inflammation in the joints.
-
RA is an autoimmune disease.
-
The goals of treatment are to relieve pain, reduce inflammation, and slow down or stop joint damage and disability.
This information is not intended to replace advice given to you by your health care provider. Make sure you discuss any questions you have with your health care provider.
 The goals of treatment are to relieve pain, reduce inflammation, and slow down or stop joint damage and disability. Treatment may include:
The goals of treatment are to relieve pain, reduce inflammation, and slow down or stop joint damage and disability. Treatment may include: If directed, apply heat to the affected area as often as told by your health care provider. Use the heat source that your health care provider recommends, such as a moist heat pack or a heating pad.
If directed, apply heat to the affected area as often as told by your health care provider. Use the heat source that your health care provider recommends, such as a moist heat pack or a heating pad.