Thoracic Outlet Syndrome Surgery
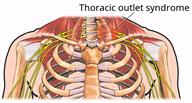
Thoracic outlet syndrome surgery consists of one or two procedures to treat thoracic outlet syndrome (TOS). TOS happens when the blood vessels or nerves are squeezed (
compressed) in the area between the collarbone (
clavicle) and lower neck. This area is called the thoracic outlet. The goal of this surgery is to reduce the pressure (
compression) that causes TOS. During TOS surgery, you may have one or both of these procedures done, depending on what is causing your TOS:
Tell a health care provider about:
-
Any allergies you have.
-
All medicines you are taking, including vitamins, herbs, eye drops, creams, and over-the-counter medicines.
-
Any problems you or family members have had with anesthesia.
-
Any bleeding problems you have.
-
Any surgeries you have had.
-
Any medical conditions you have or have had.
-
Whether you are pregnant or may be pregnant.
What are the risks?
Your health care provider will talk with you about risks. These may include:
Infection.
Bleeding.
Allergic reactions to medicines.
Damage to nearby structures or organs, such as the lungs or the nerves and blood vessels in the thoracic outlet.
Scar tissue. This may cause symptoms to return.
Symptoms of TOS getting worse.
What happens before the surgery?
Medicines
Ask your provider about:
Changing or stopping your regular medicines. These include any diabetes medicines or blood thinners you take.
Taking medicines such as aspirin and ibuprofen. These medicines can thin your blood. Do not take them unless your provider tells you to.
Taking over-the-counter medicines, vitamins, herbs, and supplements.
When to stop eating and drinking
Follow instructions from your provider about what you may eat and drink. These may include:
- 8 hours before your procedure
Stop eating most foods. Do not eat meat, fried foods, or fatty foods.
Eat only light foods, such as toast or crackers.
All liquids are okay except energy drinks and alcohol.
- 6 hours before your procedure
Stop eating.
Drink only clear liquids, such as water, clear fruit juice, black coffee, plain tea, and sports drinks.
Do not drink energy drinks or alcohol.
- 2 hours before your procedure
If you do not follow your provider's instructions, your procedure may be delayed or canceled.
Exams and tests
General instructions
- Ask your provider:
- If you will be going home right after the procedure, plan to have a responsible adult:
What happens during the surgery?
-
An IV will be inserted into one of your veins.
- You may be given:
- An incision will be made in your chest. The place where the incision will be made depends on what type of procedure is being done:
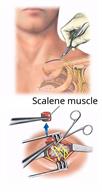
For a scalenectomy, an incision will be made just above your clavicle.
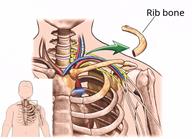
For a rib resection, an incision will be made near the thoracic outlet.
-
If you are having a scalenectomy, the scalene muscle will be cut and removed. If you are having a rib resection, the rib will be cut and removed.
-
Your incision will be closed with stitches (sutures), skin glue, or tape strips.
-
Your incision will be covered with bandages (dressings).
The procedure may vary among providers and hospitals.
What happens after the surgery?
-
You may continue to get fluids and medicines through an IV.
-
You will be given medicines for any pain.
-
Your blood pressure, heart rate, breathing rate, and blood oxygen level will be monitored until you leave the hospital or clinic.
-
You may have to wear a sling to keep your arm from moving.
-
You may be shown exercises to help your arm heal. You may be referred to a physical therapist.
This information is not intended to replace advice given to you by your health care provider. Make sure you discuss any questions you have with your health care provider.
 Thoracic outlet syndrome surgery consists of one or two procedures to treat thoracic outlet syndrome (TOS). TOS happens when the blood vessels or nerves are squeezed (compressed) in the area between the collarbone (clavicle) and lower neck. This area is called the thoracic outlet. The goal of this surgery is to reduce the pressure (compression) that causes TOS. During TOS surgery, you may have one or both of these procedures done, depending on what is causing your TOS:
Thoracic outlet syndrome surgery consists of one or two procedures to treat thoracic outlet syndrome (TOS). TOS happens when the blood vessels or nerves are squeezed (compressed) in the area between the collarbone (clavicle) and lower neck. This area is called the thoracic outlet. The goal of this surgery is to reduce the pressure (compression) that causes TOS. During TOS surgery, you may have one or both of these procedures done, depending on what is causing your TOS: